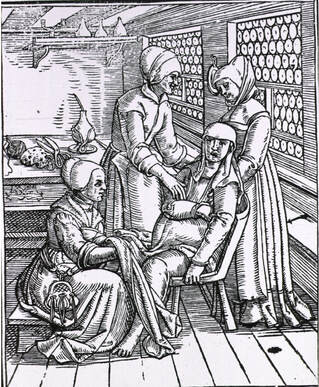
 Childbirth at Home in the 16th Century Childbirth at Home in the 16th Century The story goes like this. For centuries women gave birth at home alone or aided by other women. The late 18th and early 19th centuries saw the appearance of the so-called lying-in hospitals which began replacing home births with births at a centralized location aided by individuals trained in childbirth practices. While this change worked well initially, a terrible problem began to develop in some of these hospitals: a rise in the number of cases of puerperal fever. Puerperal fever or childbed fever was a disease that struck women after delivery. Its most common symptoms were high fevers, intense abdominal pain, and foul-smelling vaginal discharge. Although this disease was often fatal, among women who gave birth at home the fatality rate due to puerperal fever was 1% or less, whereas in some of the lying-in hospitals the fatality rate was 5-20%. Some physicians suspected that cleanliness had something to do with the disease, but none of the cleaning procedures they implemented worked. Ignaz Semmelweis was a physician appointed to serve as the head doctor in an obstetrics clinic in Vienna in 1847. The clinic had a high rate of mortality due to puerperal fever. He suspected that the disease had to do with the fact that the same doctors and students who performed examinations on pregnant women and assisted with childbirth (which included him) also performed dissections on cadavers as part of their work and studies. Although these people would wash their hands with soap and water after dissection, the smell of the corpses lingered in their hands afterwards. Semmelweis suspected that “cadaveric particles” which were transmitted from the corpses to the women by people performing dissections were to blame for the disease. Against stiff resistance, he instituted a protocol where he required anyone entering the maternity ward to clean their hands with a chlorine solution, which he found eliminated the smell from dissecting corpses. As a result of the hand-washing protocol, the rate of puerperal fever in the clinic started decreasing. Semmelweis further refined his idea to include not only transmission from corpses to patients, but transmission from sick patients to healthy ones, and instead of “cadaverous particles” he considered the origin of the disease to be any form of “decaying organic matter”. Against more opposition, he required anyone examining pregnant women to wash their hands between patients, and he succeeded in lowering the rate of puerperal fever to that of women giving birth at home. Semmelweis’s discovery was a triumph of science, and you would have expected that he would have been hailed a hero by his peers, but just the opposite happened. When he communicated his findings to the scientific community, the majority of other physicians in Europe rejected his theories and methods. He was not reappointed to his post in the clinic in Vienna and had to leave. After he left, the hand washing was discontinued and the high death toll due to puerperal fever returned. Semmelweis went on to work in the obstetric ward of a clinic in the city of Budapest where once again by instituting hand washing he was able to bring down the rate of puerperal fever. He continued trying to get his ideas accepted but met with little approval. Around 1861, Semmelweis began to develop a form of dementia and eventually had to be institutionalized. He died in an insane asylum in 1865.  Statue of Semmelweis Statue of Semmelweis It was many years later with the research of scientists such as Pasteur that the role that bacteria played in infection was understood. This led other scientists such as Lister to introduce methods of cleaning the hands and instruments of surgeons (antisepsis) to avoid infection, and these methods were then widely applied in the 1880s to maternity hospitals in Europe leading to a dramatic decline in puerperal fever. The research of Semmelweis was rediscovered in 1887, and this led to a revival of interest in his life and work. Today he is hailed as a hero and martyr. There are universities named after him, and his statues can be found in many medical institutions through the world. His valiant fight against an obtuse scientific establishment unwilling to part with old ideas has been told and analyzed in numerous books and articles. Or so the story goes, but reality is more complex. Semmelweis was a difficult man who did not deal well with rejection, and was incensed that his ideas were not accepted. He could be intolerant and dogmatic, insulting those that dared to criticize him, and he wrote angry letters to the press railing against his detractors in an egotistical and bellicose style. These character traits generated him a lot of ill-will and many enemies. Although Semmelweis published editorial accounts of his work and wrote letters to other physicians, he did not publish a formal description of his results as scientists did in those days. In the meantime, scientific descriptions of his work were mostly divulged in second or third hand accounts by students and other supporters, leading to some confusion and misinterpretations regarding the finer points of his ideas. When he did publish his results in 1861, his book was not very well written, being long, repetitive, and difficult to read, not to mention that it also contained vicious attacks against some of his critics. Additionally, at the time that Semmelweis tried to convince the medical world of his findings, there were dozens of theories that purported to explain puerperal fever, and many were championed by important and powerful personalities. Semmelweis’s theory also had several problems. For example, his emphasis on “cadaveric particles” or “decaying organic matter” as the only cause of puerperal fever could not explain why some women contracted the disease without seemingly being exposed to any of these. Finally, Semmelweis essentially claimed that doctors, by not washing their hands properly, were killing their patients, and he called many of his critics "murderers". Although this was true, it was also a very inflammatory accusation that tended to elicit an emotional rather than a rational response. There is no denying that Semmelweis made an important discovery that if widely accepted could have saved many lives, but it is painfully obvious nowadays that he torpedoed the acceptance of his ideas by his lack of tolerance and diplomacy, as well as his delay in publishing his findings and his poor writing style. His story highlights an key aspect of science that needs to be recognized by scientists that have made an important discovery that contradicts current scientific thinking. It is naïve not to take into account the complexities of human nature even in purportedly rational enterprises such as science. Evidence will not always speak for itself. To whom the evidence is presented, by whom it is presented, when it is presented, where it is presented, and how it is presented, are just as important as the nature of the evidence itself. It is not enough to be right. Engraving of three midwives attending to a pregnant woman by Jakob Rueff from the National Library of Medicine is in the public domain. Photograph by Alajos Stróbl of a marble statue of Ignaz Semmelweis in front of Szent Rókus Hospital in Budapest is from the Welcome Collection and is used here under an Attribution 4.0 International (CC BY 4.0) license. Literature consulted for this post: 1) Ignaz Phillip Semmelweis' studies of death in childbirth 2) Ignac Semmelweis (1818–1865) of Budapest and the prevention of puerperal fever 3) Ignaz Semmelweis: “The Savior of Mothers” On the 200th Anniversary of the Birth 4) Medicine in stamps-Ignaz Semmelweis and Puerperal Fever 5) Semmelweis and the aetiology of puerperal sepsis 160 years on: an historical review
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Details
Categories
All
Archives
June 2024
|
 RSS Feed
RSS Feed