|
1/29/2021 The Myth of the Unprejudiced Scientist and the Three Levels of Protection Against BiasRead Now As modern science was emerging during the 18th and 19th centuries, ideas regarding how science should be performed also began to take shape. One particular idea posited that scientists subject theories to test, but do not allow their biases to get in the way. Real scientists, it was argued, are unprejudiced, and rather than try to prove theories right or wrong, they merely seek the truth based on experiment and observation. According to this notion, real scientists don’t have preconceptions, and they don’t hide, ignore, or disavow evidence that does not fit their own views. Real scientists go where the evidence takes them. Unfortunately, the romantic notion that real scientists operate free of bias proved to be dead wrong. Scientists, even “real scientists”, are human beings, and like all human beings they have biases that influence what they do and how they do it. While a minority of scientists does engage in outright fraud, even honest scientists who claim they are only interested in the truth can unconsciously bias the results of their experiments and observations to support their ideas. In past posts I have already provided notable historical examples of how scientists fooled themselves into believing they had discovered something that wasn’t real such as the cases of the physicist René Blondot, who thought he had discovered a new form of radiation, or the astronomer Percival Lowell who thought he had discovered irrigation channels on Mars.
It is in part because of the above realization, that scientists developed several methodologies to exclude bias and limit the number of possible explanations for the results of experiments and observations such as the use of controls, placebos, and blind and double-blind experimental protocols. This is the first level of protection against bias. Today the use of these procedures in research is pretty much required if scientists expect their ideas to be taken seriously. However, while nowadays scientists use and report using the procedures described above when applicable, the proper implementation of these procedures is still up to the individual scientists, which can lead to biases. This is where the second level of protection against bias comes into play. Scientists try to reproduce each other’s work and build upon the findings of others. If a given scientist reports an important finding, but no one can reproduce it, then the finding is not accepted. But even with these safeguards, there is still a more subtle possible level of bias in scientific research that does not involve unconscious biases or sloppy research procedures carried out by one or a several scientists. This is bias that may occur when all the scientists involved in a field of research accept a certain set of ideas or procedures and exclude other scientists that think or perform research differently. Notice that above I used the words “possible” and “may”. The development of a scientific consensus within the context of a well-developed scientific theory always leads to a unification of the ideas and theories in a given field of science. So far from bias, this unification of ideas may just indicate that science has advanced. But in general, and especially early on in the development of a scientific field, science is best served not when researchers agree with each other but when they disagree. So the third level of protection against bias that keeps science true occurs when researchers disagree and try to prove each other to be wrong. In fact, some funding agencies may even purposefully support scientists that hold views that are contrary to those accepted in a field of research. The theory is that this will lead to spirited debates, new ways of looking at things, and a more thorough evaluation of the thinking and research methods employed by scientists. However, disagreements among scientists do have a downside that is often not appreciated. While science may benefit when in addition to Scientist A, there is a Scientist B researching the exact same thing who disagrees with the ideas and theories of Scientist A, science may not necessarily benefit when Scientist A and B research something and A thinks that B is wrong and doesn’t have the slightest idea of what he/she is doing, while B thinks A is an idiot who doesn’t understand “real science”. There are a number of examples of long-running feuds in science between individual scientists or even whole groups of scientists. In these feuds, the acrimony can become so great that the process of science degenerates into dismissal of valid evidence, screaming matches, insults, and even playing politics to derail the careers of opponents. But, of course, the problem I have described above is nothing more than the human condition and in this sense science is not unique. Every activity where humans are involved has to deal with bias, but at least in science we can recognize we are biased and implement the three levels of protection against this bias. It may be imperfect, it may be messy, it may not always work, but, being human, that’s the best we can do. Image from Alpha Stock Images by Nick Youngson used here under an Attribution-ShareAlike 3.0 Unported (CC BY-SA 3.0) license.
0 Comments
 The Raising of Lazarus The Raising of Lazarus The drug hydroxychloroquine is being tested against COVID19, but there is still no compelling scientific evidence that it works, let alone that it is a “game changer” in our fight against COVID19. However, the president has claimed that there are very strong signs that it works on coronavirus, and the president’s economic adviser, Peter Navarro, has criticized the infectious disease expert, Dr. Anthony Fauci, for questioning alleged evidence hydroxychloroquine works on COVID19. The French researcher, Dr. Didier Raoult, who performed the original trial of hydroxychloroquine that generated all the current interest in the drug, now claims that he has treated 1,000 patients with COVID19 with a 99.3% success rate. In the news, I have read descriptions of patients that have recovered after being administered hydroxychloroquine in what has been called a “Lazarus effect” after the Biblical story where Jesus brought Lazarus back from the dead. So what is a scientist to make of this? I have acknowledged that science cannot operate in a vacuum. I recognize something that Dr. Fauci has also recognized, and that is that people need hope. However, as Dr. Fauci has also stated, scientists have the obligation to subject drugs to well-designed tests that will conclusively answer the question of whether a drug works or not. There seems to be a discrepancy between the quality of the evidence that scientists and non-scientist will accept to declare that a drug works, and there is the need to resolve this discrepancy. People anxiously waiting for evidence regarding whether hydroxychloroquine works, will understandably concentrate on patients that recover. Therefore they are more prone to make positive information the focus of their attention. Any remarkable cases where people recover (Lazarus effects) will invariably be pushed to the forefront of the news, and presented as evidence that the drug works wonders. What people need to understand, is that these “Lazarus” cases always occur, even in the absence of effective interventions. We all react to disease and drugs differently. Someone somewhere will always recover sooner and better than others. How do we know whether one of these Lazarus cases was a real effect of the drug or a happenstance? Isolated cases of patients who get better, no matter how spectacular, are meaningless. Scientists look at people who recover from an illness after being given a drug in the context of the whole population of patients treated with the drug to derive a proportion. The goal is then to compare this proportion to that of a population of patients not given the drug. Scientists also have to consider both positive and negative information. For the purposes of determining whether a drug works, patients that don’t recover are just as important to take into account as those that do. What if a drug benefits some patients to a great extent but kills others? Depending on the condition being treated, it may not be justified to use this drug until you can identify the characteristics of the patients that will be benefited by the drug. To do all the above properly, you need to carry out a clinical trial. No matter how desperate people are, and no matter how angry it makes them to hear otherwise, this is the only way to establish whether a drug works or not. 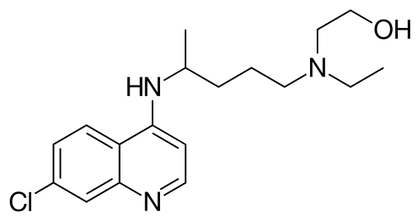 Hydroxychloroquine Hydroxychloroquine Once we accept the need for a clinical trial to establish whether a drug works, another issue is trial design. A trial carried out by scientists is not valid just because it happened. There are optimally-designed trials and suboptimal or poorly designed trials. There are several things a optimally designed trial must have. 1) The problem with much of the evidence regarding hydroxychloroquine is that it has been tested against COVID-19 in very small trials, and clinical trials of small size are notorious for giving inaccurate results. You need a large enough sample size to make sure your results are valid. 2) Another problem is: what you are comparing the drug against? Normally, you give the drug to a group of patients, and you compare the results to another group that simultaneously received an inert dummy pill (a placebo), or at least to a group of patients that received the best available care. This is what is called a control group. In many hydroxychloroquine trials there were no formal control groups, but rather the results were loosely compared to “historical controls”, in other words, to how well a group of patients given no drug fared in the past. But this procedure can be very inaccurate as there is considerable variation in such controls. 3) Another issue is the so called placebo effect. The psychology of patients knowing that they are being given a new potentially lifesaving drug is different from that of patients that are being treated with regular care. Just because of this, the patients being given the drug may experience an improvement (the so called placebo effect). To avoid this bias, the patients and even the attending physicians and nurses are often blinded as to the nature of the treatment in the best trials. Most hydroxychloroquine studies were not performed blind. 4) Even if you are comparing two groups, drug against placebo or best care, you need to allocate the patients to both groups in a random fashion to make sure that you do not end up with a mix of patients in a group that has some characteristic that is overrepresented compared to the other group, as this could influence the results of the trial. Most hydroxychloroquine studies were not randomized. These are but a few factors to consider when performing a trial to determine whether a drug works. These and other factors, if they are not carefully dealt with, can result in a trial yielding biased results that may over or underestimate the effectiveness of a drug. Due to budget constraints, urgency, or other reasons, scientists sometimes carry out very preliminary trials that are not optimal just to give a drug an initial “look see” or to gain experience with the administration of the drug in a clinical setting. But these trials are just that, preliminary, and there is no scientific justification to base any decision regarding the promotion of a drug based on this type of trials. The FDA recently has urged caution against the use of hydroxychloroquine outside the hospital setting due to reports of serious heart rhythm problems in patients with COVID-19 treated with the drug. A recent study with US Veterans who were treated with hydroxychloroquine found a higher death rate among patients who were administered the drug (to be fair, this study was retrospective and therefore did not randomize the allocation of patients to treatments, so this could have biased the results). Even though I am skeptical about this drug, I would rather save lives than be right. I really hope it works, but the general public needs to understand that neither reported Lazarus effects nor suboptimal clinical trials will give us the truth. The 1310-11painting The Raising of Lazarus by Duccio di Buoninsegna is in the public domain. The image of hydroxychloroquine by Fvasconcellos is in the public domain.  There is a joke that illustrates misguided science thinking. A man is in a public area screaming at the top of his lungs. When somebody comes over and enquires why he is screaming, the man replies, “To keep away rogue elephants”. When told that there are no elephants for miles around, the man replies that this is proof his screaming is working. If you think that is silly, consider the following recipe for obtaining mice by spontaneous generation (in other words, without the need for male and female mice): Place a soiled shirt into the opening of a vessel containing grains of wheat. Within 21 days the reaction of the leaven in the shirt with the fumes from the wheat will produce mice. No, I’m not kidding you! For many centuries some of the best minds in humanity believed that life could regularly arise spontaneously from nonlife or at least from unrelated organisms. Some people went as far as outlining procedures to achieve this, such as the one presented above to generate mice supplied by the chemist Jean Baptiste van Helmont. Presumably, this individual (who is no stranger to misguided scientific thinking) placed a shirt in a vessel with grains of wheat, and when he checked 21 days later he saw a mouse scurrying away. Therefore, he concluded that the mix of the wheat and the shirt in the vessel produced the mouse. What the above examples of misguided science have in common is the ignoring of alternative explanations. In the case of the joke, the alternative explanation obviously is that there are no rogue elephants nearby to begin with. In the other case, the alternative explanation is that the mouse came from elsewhere, as opposed to arising from the shirt with the wheat. The best scientific experiment is one carried out in such a manner that alternative explanations for the experimental results are minimized or ruled out altogether. The ideal scientific experiment should only have one possible explanation for the outcome. In order to achieve this, scientists use controls. A control is an element of the experimental design that allows for the control of variables that could otherwise affect the outcome of the experiment. In the case of the joke, the man could stop screaming to see if rogue elephants show up, or he could scream next to an actual elephant to see if screaming works. In the case of the real example, van Helmont could have placed a barrier around the shirt with the wheat to rule out that mice came from the outside. The use of controls in experiments is so commonplace nowadays, that it is really hard to imagine how anyone could even think of performing an experiment without them. However, the modern universal notion of controls as a way of controlling variables to rule out alternative explanations to experimental results did not begin to take shape until the second half of the 19th century, even though scholars claim that strategies to make observations or experiments yield valid results go back further in time to the Middle Ages or even antiquity. In science, the controls that are most often used are those involving outside variables that can affect the results of an experiment. However, the more important and more challenging variables to control are those that arise from within the experimenter.  Illustration of the Canals on Mars by Percival Lowell Illustration of the Canals on Mars by Percival Lowell If the procedure to make an observation or evaluate the results of an experiment depends on a subjective judgement made by the experimenter, as opposed to, for example, a reading made by a machine, then subtle (and not so subtle) psychological factors can influence the result depending on the biases of the experimenter. I have already mentioned the famous case of the scientist René Blondlot who in 1903 announced to the world he had discovered a new form of radiation (N-rays), but it turned out that such radiation existed only in his imagination. Another famous case was that of astronomer Percival Lowell who, at the turn of the 19th century, thought he saw canals on Mars which he considered to be evidence of an advanced civilization. He was a great popularizer of science and he wrote several books about Mars and its inhabitants based on his observations, but the whole thing turned out to be a delusion. To avoid this type of mistake, many experiments that rely on subjective assessments employ a protocol where the observer does not know which groups received which treatments. This is called a blind experimental design.
An additional challenge occurs when a scientists works with human subjects. Psychological factors can have a potent role in influencing the results of medical experiments. Depending on the disease, if patients are convinced that they are receiving an effective treatment, and that their condition will improve, said patients can display remarkable improvements in their health even if they have received no effective treatment at all. To rule out the effect of these psychological factors, scientist performing clinical trials include groups of patients treated with placebos. Placebos are fake pills designed to mimic the actual pill containing the active chemical substance or ineffective procedures designed to mimic the actual medical procedure in such way that the patient cannot tell the difference. To also rule out the influence of psychological factors arising from the doctors giving patients in one group a special treatment, the identity of these groups are hidden from the clinicians. Clinical trials which employ placebos and where both the patients and the clinicians don’t know the identity of the treatments, are called double-blind placebo-controlled trials, and they are the most effective and also the most complex forms of controls. Unfortunately, the use of controls is not always straightforward. I have already mentioned the case of the discovery of polywater which was heralded as a new form of water with intriguing properties that promised many interesting practical applications until someone implemented a control and demonstrated that it was the result of contamination. Sometimes scientists do not know all the variables affecting an experiment, or they may underestimate the effect of a variable that they have deemed irrelevant, or they may misjudge the extent to which their emotional involvement in conducting the experiment may compromise the results. Designing the adequate controls into experimental protocols requires not only discipline, discernment, and smarts, but sometimes also just luck. In fact, some scientists would argue that implementing effective controls is not a science but an art. The art of the control! The Elephant cartoon from PixaBay is free for commercial use. The Illustration of Mars and its canals by Percival Lowell is in the public domain. In the late 19th century a series of remarkable discoveries in physics were made including X-rays and radioactivity. A new world of physical phenomena was being uncovered by scientists, and hopes of new discoveries were high. It was thus in 1903 that the French physicist Prosper-René Blondlot announced that he had discovered a new form of radiation which he christened N-rays after the University of Nancy where he worked. The problem was that N-rays were difficult to detect and several scientists had problems reproducing Blondlot’s experiments. So the British Journal Nature sent the physicist Robert Wood to Blondlot’s lab to witness an N-ray demonstration.  The demonstration involved an N-ray producing machine that relied on a prism made of aluminum to generate the rays. The room was darkened, the machine was started, and the N-ray measurements were begun. But Wood, who had a reputation as a debunker, removed the prism from the machine - something that would have caused the N-rays to cease to be produced. However, Blondlot and his assistant kept making the N-ray readings as if nothing had happened. This and other evidence led Wood to conclude that this radiation did not exist, and that what Blonlot was detecting was only present in his imagination. The N-ray story is a classic example of experimenter bias. When a scientist is performing measurements that involve a subjective component, there is the danger that the scientist will see what he or she wants to see. The common solution to this problem is to make the scientist blind. Thankfully this does not involve gouging their eyes out, but rather coding the samples to be evaluated. In this way the experimenter is “blind” to the identity of the samples and thus the bias is eliminated. These blind protocols are routinely applied in science whenever there is a chance that knowing the identity of the samples will affect their reading. But the complexity of the human mind to warp the scientific enterprise goes beyond the laboratory. In clinical trials a very well-known phenomena is the placebo effect. In this effect the patient experiences an improvement in their condition after being administered an inert substance or exposed to a procedure that should not be effective at treating their ailment. To avoid experimenter bias and the placebo effect, clinicians implement what is called a double blind protocol where both the doctor and the patient do not know the identity of the treatment. Not controlling experimenter bias can lead to bad science. So, you see, the only good scientist is a blind scientist! The image from Archive.org is in the public domain. |
Details
Categories
All
Archives
June 2024
|
 RSS Feed
RSS Feed